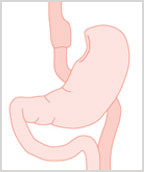
The Procedure:
A surgical stapling device divides and seals the upper stomach to create a new, smaller stomach pouch. The pouch is about the size of an egg yolk and holds 15 ml or less. The stomach pouch is attached to a segment of the small intestine (the Roux limb), which carries food downstream for digestion. With the new smaller pouch, patients find that they can eat much less and still feel satisfied. More importantly, the Gastric Bypass causes a significant GI hormone “rebalancing” that leads to a smaller appetite and improvement in many medical conditions. About 99% of the time, we do this procedure laparoscopically. Patients spend 1-3 nights in the hospital, and recovery time is usually 1-2 weeks.
The Results:
The gastric bypass has a history of success dating back to the early 1980′s. Among common bariatric procedures, the gastric bypass is the best studied has excellent long term weight loss results with the minimum amount of long term complications. Gastric bypass is the gold standard for weight loss surgery. The gastric bypass is particularly effective for patients with diabetes and GERD (reflux).
Additional Considerations:
One special effect of this surgery is that the intestine can no longer handle concentrated sugars or starches. If a patient consumes sweets or starchy foods, they have a temporary illness called Dumping Syndrome. While it’s not dangerous, the unpleasant symptoms include nausea, a “clammy” feeling, palpitations, vomiting, diarrhea and weakness. Dumping syndrome is actually one of the helpful features that helps steer Gastric Bypass patients away from sweets. Dumping Syndrome is not something that randomly happens – concentrated sugar – has to be ingested before it sets off the cascade. It usually lasts for 30-45 minutes and is very effective at keeping patients away from high carbohydrate foods. For most patients, taking in less than 10-14 grams of carbohydrates per serving is safe.