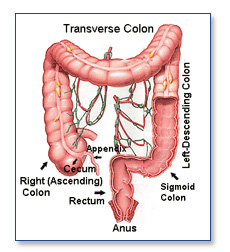
The colon or large bowel is the part of the intestine that transfers waste material from the small bowel to the rectum. Removal or resection of a portion of the colon (or the entire organ) can be indicated for infectious or inflammatory problems, such as complications of diverticulitis and ulcerative colitis, poor blood supply, bleeding lesions, polyps, and cancers.
Most pathology in the colon is diagnosed by the results of procedures including colonoscopy, barium enema, computed tomography (CT scan).
Treatment
Traditionally, a colon resection was performed with a long midline abdominal incision. Patients would spend a week or more in the hospital and not able to return to normal activities for at least six weeks after surgery. However, laparoscopic colectomy is the technique of using the laparoscope for surgical removal of a portion of the colon. This is a relatively new addition to the range of procedures that are carried out using minimally invasive techniques. As a result of a large clinical trail, the Society of American Gastrointestinal and Endoscopic Surgeons, as well as the American Society of Colon and Rectal Surgeons, have approved the use of laparoscopic colon resection for the treatment of colon and rectal cancer.
Surgery
Before and After
In preparation for laparoscopic colectomy, the patient is asked to completely clean the bowel. Four to six tiny incisions are made, and through these incisions, a camera and instruments are placed into the abdomen. One larger incision is made to bring out the colon.
The colon and its blood supply are divided, using a combination of staples and clips. Once the dissection is complete, the colon is extracted through one of the incisions and removed. The anastomosis (re-connect) is then done and the bowel returned to the abdominal cavity.
The advantages of laparoscopic colectomy and laparoscopically-assisted colectomy include smaller incisions, less pain, shorter recovery, quicker return of bowel function, quicker return to normal activity and a better cosmetic result.
The preoperative period
Your SCOSA surgeon will review with you the risks and benefits of the procedure at your clinic appointment. You will be sent for some routine lab work, X-rays, and an EKG. In addition, your SCOSA surgeon will set up any further testing required to evaluate your colon before surgery.
On the day before surgery, you should have only a clear liquid diet and nothing to eat or drink after midnight with the exception of some medications. In addition, you will be given a special bowel preparation to clean your colon for the operation. This process will be explained by your SCOSA surgeon. You should shower the day before or the morning of your operation.
Medications such as aspirin, coumadin, or other blood-thinning agents should be stopped at least seven days prior to surgery. Vitamin E, diet medications and St. John’s Wort should also be stopped at least one week prior to surgery.
Please go over any specific questions with your SCOSA surgeon.
Patients are encouraged to stop smoking and begin an exercise program in advance of any operation.
The day of operation
Your SCOSA doctor will give you detailed instructions about where and when you should be the morning of your surgery.Once you arrive at the hospital, a nurse will start an IV, and you will meet with your anesthesiologist and your SCOSA surgeon to answer any last-minute questions. You will likely receive some pre-operative medications and then be taken to the operating room.
After surgery, you will be in the recovery room until you are completely awake. Your room will include a breathing device called an incentive spirometer. It is important that you use this several times each hour when you are awake. The nurses on the floor will give you specific instructions about its use. In addition, it is important that you get out of bed and walk in the hall. We like our patients to do this at least once the afternoon after surgery and then at least four times each following day. These activities are vitally important to prevent a blood clot from forming in your legs, pulmonary embolism, breathing problems, and pneumonia.
After-effects of Surgery
Most patients spend three to four nights in the hospital. You will be given a prescription for pain medication and specific discharge instructions. You will be able to shower beginning the second day after your surgery. You should follow up with your SCOSA surgeon two weeks after the operation.
Although this operation is very safe and has a less than 1 percent mortality rate, this is an important decision for you and your physician. Potential acute complications are rare, but can include bleeding, infection, damage to bowel, ureters (the tube which carry urine from the kidney to the bladder), bladder or internal organs. Other less common risks are hernia, wound problems, need for open surgery or re-operation. Leaks from the anastomosis or fistula can rarely occur. In any colon operation, the need to perform a colostomy (diverting the stool to a bag placed on the outside of the abdominal wall) is always a possibility, albeit remote, consideration. Narrowing or stricture of the anastomosis is also a rare complication. You should call your SCOSA surgeon immediately if you experience any of the following after this procedure: persistent fever of more than 101 degrees, persistent nausea or vomiting; worsening abdominal pain- uncontrolled by medication; increasing abdominal swelling; chest pain; shortness of breath; redness around or pus coming from incisions; or the inability to tolerate liquids.
Following a laparoscopic surgery, patients usually stay in the hospital for 3-4 days – compared to 5-8 days for an open procedure. Patients are able to return to normal activity in one or two weeks. The technical demands of the laparoscopic procedure require a high level of training and expertise.
Outcomes
Most patients have complete resolution or a significant improvement of their symptoms.